 Understanding Benefit Programs
Understanding Benefit ProgramsThis chapter provides an overview of benefit programs and discusses how to:
Build benefit programs.
Clone benefit programs, eligibility rules, or event rules.
 Understanding Benefit Programs
Understanding Benefit ProgramsThis section provides an overview of:
Benefit programs.
Plan types.
Plans.
Effective dates.
See Also
Building Automated Benefit Programs

 Understanding Benefit Programs
Understanding Benefit Programs
A benefit program is a collection of benefits that are offered to a group of employees. You may have multiple benefit programs if you offer different benefits to different groups of employees, charge different premiums, or administer enrollment rules differently for various employee groups.
Use the Benefit Program Table to establish a program for employees, link the appropriate plan types and benefit plans to it, and associate a variety of rules, such as rates and calculation rules. The Benefit Program Table brings together all of the information that relates to a benefit program, including whether to process enrollments manually or use PeopleSoft Enterprise Benefits Administration automated enrollment. This table shows the building blocks for benefit programs:
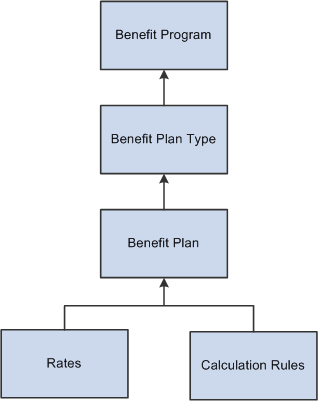
Building blocks for benefit programs

 Understanding Plan Types
Understanding Plan Types
Plan types are essential in a benefit program. They group individual plans or options that can be elected by an employee for a particular type of benefit, such as basic life insurance or medical.

 Understanding Plans
Understanding Plans
Plans are the individual benefits into which an employee can be enrolled. A plan is always subordinate to a plan type. For example, you may offer employees a choice of four different medical plans, each from a different HMO (health maintenance organization) or plan provider. In this case, you would be offering four different plans in the medical plan type. Each plan has an associated deduction code, set of rates, and calculation rules.

 Understanding Effective Dates
Understanding Effective Dates
To keep your benefit program accurate and consistent, the benefit plans, calculation rules, and options must be individually effective-dated in a coherent, logical manner. If they aren't, your benefit program will be left open to a variety of errors.
Using effective dates is an efficient way for you to maintain accurate records of your benefits information. You can create historical records and enter future-dated information at your convenience, all because when you enter information, you also enter an effective date that is synchronized with the effective dates for the other elements of the benefit program.
Provider and Benefit Plan Effective Dates
Consider provider and benefit plan information. To set up a provider, enter its effective date on the Provider table. To set up a benefit plan, enter the plan's effective date and identify its provider on the Benefit Plan Table. The system checks that the provider is effective prior to or on the same date as the benefit plan; otherwise, the provider information cannot exist for the benefit plan.
Benefit Programs and Effective Dates
Things get more complicated when you associate a set of rates and calculation rules, which also have effective dates, with a benefit program and its associated benefit plans. The system reviews the effective dates of the program, the plan, the rates, and the calculation rules. The system can't check that you've set up the correct dates, because any date could possibly be correct. Instead, it goes by the benefit program.
The system looks for effective dates for the benefit program that you're working with and the set of benefit plans that you associate with that benefit program. A benefit program and benefit plan combination is effective based on both sets of dates.
Plans associated with a benefit program can't be in effect unless their effective dates are set on or before the effective date of the benefit program. Similarly, the rates and calculation rules that you associate with the plans can't be in effect unless their effective dates are set on or after the dates of their respective plans.
If a benefit program and benefit plan combination is not effective when you think it should be and your plan does not appear, check the effective dates of the benefit program and the benefit plan. The effective date of the benefit plan must be earlier or the same as the effective date of the benefit program.
Loading History: A Warning
When you're setting up tables, you must set effective dates to reflect when you want the data to go into effect. If you load employee history, make sure that you establish an early effective date. When preparing for a conversion, set all effective dates to the same date. Most tables also have a status, which you would normally leave as Active.
 Building Benefit Programs
Building Benefit Programs
To define benefit programs, use the Benefit Program Table (BEN_PROG_DEFN) component.
This section discusses how to:
Define basic benefit program information.
Associate plan types with a benefit program.
Link a benefit program and plan type to rate and calculation rules.

 Pages Used to Build Benefit Programs
Pages Used to Build Benefit Programs|
Page Name |
Definition Name |
Navigation |
Usage |
|
BEN_PROG_DEFN1 |
Set Up HRMS, Product Related, Base Benefits, Program Structure, Benefit Program Table, Benefit Program |
Define basic benefit program information. |
|
|
BEN_PROG_DEFN2 |
Set Up HRMS, Product Related, Base Benefits, Program Structure, Benefit Program Table, Plan Type and Option |
Link plan types to the benefit program and add important information about plan types. |
|
|
BEN_PROG_DEFN3 |
Set Up HRMS, Product Related, Base Benefits, Program Structure, Benefit Program Table, Cost |
Link a benefit program and plan type to rate and calculation rules. |

 Defining Basic Benefit Program Information
Defining Basic Benefit Program Information
Access the Benefit Program Table - Benefit Program page (Set Up HRMS, Product Related, Base Benefits, Program Structure, Benefit Program Table, Benefit Program).
|
Effective Date |
The date the row in the table becomes effective. This date determines when you can view and change information. |
|
Status as of Effective Date |
Indicates whether a row in the table is Active or Inactive. Processes ignore benefit programs designated as Inactive, even if the effective date defines the program as current. |
|
Program Type |
The type of program can be Manual or Automated. If you are using only the Manage Base Benefits business process, this option is automatically set to Manual. If you activate Benefits Administration on the Installation Table, it is automatically set to Automated. |
|
Currency Code |
The type of currency that is used for this program's benefit and deduction calculations. |
Dependent Limits
This group box defines the age at which dependents are no longer eligible for health benefits.
|
Dependent Age Limit and Student Age Limit |
Defines the age at which a dependent is no longer considered to be a dependent or a student. |
|
Exclude Disabled from Age Lmt. (exclude disabled from age limit) |
Select to exclude disabled dependents from the age limits. |
|
Dep Ineligible if Married (dependent ineligible if married) |
Select to consider married dependents ineligible for health benefits, regardless of their age. |
Benefits Administration
This group box is available if Benefits Administration is activated on the Installation Table. If you are using flexible credits, it is used to define how the system will process excess flexible credit amounts when an employee does not designate a rollover election during benefit enrollment.
|
Apply Excess Credits to |
The system can convert excess flexible credit amounts to: C (Cash) D (FSA-Dependent Care) F (Forfeit Excess Credit) H (FSA-Health Care) R (FSA Retirement Counseling) S (Savings-401(k)) |
FSA
For FSA (flexible spending account) Administration users. Use this group box to set up your organization's business rules for flexible spending accounts.
|
Flexible Spending Acct Run ID (flexible spending account run ID) |
For FSA Administration users. Enter the FSA run ID that you created on the FSA Run Table. |
|
FSA Maximum Annual Pledge |
Enter the maximum amount that an employee can pledge to deposit into a flexible spending account. |
COBRA
This group box defines the rules regarding the surcharge amounts that your organization imposes on COBRA (Consolidate Omnibus Budget Reconciliation Act) plans.
|
COBRA Surcharge % (COBRA surcharge percentage) |
Enter the percentage amount of the benefit cost that you want added to the benefit cost. For example, if the cost of medical coverage is 100 USD and the COBRA surcharge % is 30%, the cost for medical coverage for someone on COBRA would be 130 USD. |
|
COBRA Disabled Surcharge % (COBRA disabled surcharge percentage) |
If you want a different percentage amount for a disabled person, enter that percentage amount. If you leave the field blank, the surcharge amount entered in the COBRA Surcharge % field will be applied to a disabled person with COBRA coverage. |
Self-Service Configuration
Use this group box to define the rules for displaying and processing the PeopleSoft Enterprise eBenefits application pages.
|
Show Credits on Enrollmnt Form (show credits on enrollment form) |
Select if you want credit amounts to appear on the enrollment form. If you do not offer flexible credits, you may not want this heading to appear on the form. |
|
Include Can Sales Tax on Form (include Canadian sales tax on form) |
Select if you want Canadian sales tax information to appear on the eBenefits Enrollment Summary page. |
|
Show Employer Costs on Form |
Select to display the employer's contributions (costs) on the enrollment form |
|
Alert to Tax Impacts on Form |
Select to alert the employee to any potential tax impacts (due to the employer's contributions) on the enrollment form. Most typically, this would be if a T-Tax (imputed income) component existed. |
|
Cost Freq on Enrollment Form (cost frequency on enrollment form) |
This defines how the cost of the benefits appears on the enrollment form. Values are Annual: Displays the costs as annual amounts. Deduction: Displays the costs as per-pay-period amounts. |
|
Handbook URL ID (handbook uniform resource locator identification) |
Enter the URL ID that connects to your benefit handbook. URL IDs are set up in the URL Table. |
FMLA
Use this group box to define the rules for processing under FMLA (Family Medical Leave Act).
|
FMLA Plan ID (FMLA plan identification) |
Enter the FMLA plan ID that you created on the FMLA Plan Table. |
See Also

 Associating Plan Types with a Benefit Program
Associating Plan Types with a Benefit Program
Access the Benefit Program Table - Plan Type and Option page (Set Up HRMS, Product Related, Base Benefits, Program Structure, Benefit Program Table, Plan Type and Option).
|
Plan Type |
Select the plan type that you want to add or display. |
|
DispPlnSeq (display plan sequence) |
For Benefits Administration users. Indicates the order in which benefit plans appear. The default value is the plan type. |
|
Event Rules ID |
For Benefits Administration users. Select an event rule that you want to link to this benefit plan. Event rules are set up on the Event Rules Table. |
|
HIPAA Plan (Health Insurance Portability and Accountability Act plan) |
This check box applies only to health plans. Select this check box if you want to designate that this plan be included in the HIPAA Report. |
|
Waive Coverage |
For Benefits Administration users. Select the option that defines whether and when employees are permitted to waive coverage for this plan type. |
|
COBRA Plan |
Select to designate which health plan types (limited to Plan Types 1x and 60) are COBRA-qualified plan types. If you make this plan type COBRA-qualified, enter an option code for each of your plans. Otherwise, the Option Code field will be unavailable. |
|
Load Cross Plan Values |
Click to automatically supply the cross-plan data for every option in this plan type. For Benefit Administration users only. |
Self-Service Configuration
Use this group box to define the rules for displaying enrollment and plan information on the eBenefits pages.
|
Collect Dependent/Beneficiary |
Select this check box when you want the system to collect information pertaining to dependents and benefits and display that information on the eBenefit Summary and the eBenefit Detail Information pages. This works in conjunction with the Ignore Dep/Ben Edits check box on the Event Rules page. |
|
Collect Fund Allocations |
When this check box is selected, the system collects the information pertaining to savings plans and displays that information on the eBenefit Savings Summary and the Detail Information pages. |
|
Show if no choice |
This check box controls whether a plan type appears on the enrollment when the employee has no option to choose and cannot waive out of the option. A good example is paid vacation. Employees receive the benefit, but you don't display it on the enrollment form. If the check box is selected, the system displays the plan type in the enrollment form summary. When the check box is deselected, the system will not display the plan type. |
|
Handbook URL |
If you have a special handbook for this plan type, you can enter the URL ID. URL IDs are set up in the URL Table. |
Option – Eligibility Tab
Enter the options that are available to the employee for the designated plan type in this section.
|
Optn ID (option ID) |
As you define options for each of the plan types that are offered, the system automatically enters the option ID. |
|
Optn Type (option type) |
Each option row needs to have an option type designation. The Manage Base Benefits business process enables you to select from the following list of values: O: At least one option is required per plan type, except for plan type 01. Plan type 01 is used only for Benefits Administration. It is also called the Program level of the benefits program and is used only by programs that run in conjunction with Benefits Administration. G: Designates that this option is a general credit and used only in Benefits Administration. P: This is used only for plan type 01. It designates that this is a program and is required for automated benefit programs. Only one P row is allowed per benefit program. W: Designates that waiving coverage is an option and is used only in Benefits Administration. |
|
Benefit Plan |
Enter the code for a benefit plan that was defined on the Benefit Plan Table. If it is something other than a health plan, provide added detail in one of the various benefit plan detail pages. |
|
Covrg Code (coverage code) |
This applies only to health plan types. Indicate the level of coverage for health plans. This is a required field for those plan types. Coverage codes are defined on the Coverage Code Table. |
|
Deductn Cd (deduction code) |
Links the deduction code to the option. |
|
Option Code |
This field is available if the COBRA Plan check box is selected, or if this is a Benefits Administration (Automated) benefit program. |
|
Default Option |
Applies to Benefits Administration. Select this check box if you want this option to be used as the default when the Benefits Administration process validates, loads, or finalizes participant elections. The default option is the benefit plan option that is given to employees who do not make an election and is used if the associated event rule has a default method of Option or Current Else Option. Plan type defaults are used as substitutes for a participant's election when you finalize the event. Here are some guidelines for setting default options:
|
|
Opt Level (option level) |
Applies to Benefits Administration. Option level refers to the level of benefits coverage provided by the option. For example, suppose you're setting up a set of supplemental life options that will enable employees to choose a coverage of 1, 2, 3, or 4 times their annual salary. Set option level values for these options of 1, 2, 3, and 4, respectively. The option level values are used by the system during event processing. The event rule, linked to the plan type to which these options belong, checks the option level when evaluating its change level rules. When an employee elects new coverage, the system compares the option level of the employee's new option election in that plan type with the employee's current option election. If the new election violates the associated event rule's Participate and Waive change level rules, the system rejects the employee's benefit option selection. If, for example, the associated event rule's maximum number of change levels is 2, the system prevents employees from changing their coverage more than two option levels in either direction. Therefore, an employee with coverage equal to 1 times her annual salary would not be allowed to select coverage equal to 4 times her annual salary during open enrollment. |
|
Option Seq (option sequence) |
Applies to Benefits Administration. Indicates the order in which benefit options appear. The default value is the plan type. |
|
Geog Locn (geographic location) |
Applies to Benefits Administration. If you want to link a geographic location rule to this option, enter the code. Geographic location rules are set up on the Geographic Location Table. |
|
Elig ID (eligibility ID) |
Applies to Benefits Administration. If you want to link an eligibility rule to this option, enter the eligibility rule ID. Eligibility rules are created on the Eligibility Rules Table. |
Option – Cross Plan Tab
This tab is only for Benefit Administration users.
|
Optn ID (option identification) |
As you define options for each of the plan types that are offered, the system automatically enters the option ID. |
|
Covrg Code (coverage code) |
This applies only to health plan types. Indicate the level of coverage for health plans. It is a required field for those plan types. Coverage codes are defined on the Coverage Code Table. |
|
Deductn Cd (deduction code) |
Links the deduction code to the option. |
|
Option Code |
Displays the information created in the Eligibility section. |
|
Cross Plan Type |
If a cross-plan requirement exists for this option, enter the other plan type that must have an enrollment. |
|
Cross Benefit Plan |
This field is for automated benefit programs and indicates that enrollment in this option depends upon enrollment in a particular benefit plan entered in the Cross-Plan Type field. |
|
Coverage Limit |
This field is for automated benefit programs and indicates that coverage is limited to a percentage of the employee's coverage amount in the other plan type. |
|
Check Dependents |
This field is for automated benefit programs and tells the system to check the dependent's enrollment in this plan against the dependent enrollments in the other plan type. |
The following chart shows you how to fill out the Plan Type and Option page for plan types 01 through 9x:
|
Field |
Value for Plan Type 01 |
Value for Plan Types 1x–9x |
|
Plan Type |
01 (Plan type 01 not allowed within Base Benefits) |
1x−9x |
|
Display Plan Sequence |
NA |
Not allowed |
|
Event Rules ID |
NA |
Not allowed |
|
Waive Coverage |
NA |
Not allowed |
|
COBRA Plan |
NA |
Allowed for plan types 1x and 6x |
|
HIPAA Plan |
NA |
Allowed for 1x plan types |
|
Option Type |
NA |
O - Only option type allowed for plan types 1x–9x |
|
Benefit Plan |
NA |
Required |
|
Coverage Code |
NA |
Required for plan type 1x, Not allowed for plan types 2x–9x |
|
Default Option Indicator |
NA |
Not allowed |
|
Deduction Code |
NA |
Required |
|
Option Sequence |
NA |
Not allowed |
|
Option Code |
NA |
Not allowed, unless plan type 1x or 60 has been designated as a COBRA plan, in which case the option code is required. |
|
Option Level |
NA |
Not allowed |
|
Geographic Location Table ID |
NA |
Not allowed |
|
Eligibility Rules ID |
NA |
Not allowed |
|
Cross-PlanType |
NA |
Not allowed |
|
Cross-Plan |
NA |
Not allowed |
|
Cross-Plan Limit Percentage |
NA |
Not allowed |
|
Cross-Plan Dependent |
NA |
Not allowed |
Note. NA stands for "not applicable".
See Also

 Linking a Benefit Program and Plan Type to Rate and Calculation Rules
Linking a Benefit Program and Plan Type to Rate and Calculation Rules
Access the Benefit Program Table - Cost page (Set Up HRMS, Product Related, Base Benefits, Program Structure, Benefit Program Table, Cost).
Cost
Use this group box to identify the rate and calculation rules for each benefit program and option combination.
|
Cost Type |
Identifies the cost type for this plan type and benefit option combination. For Base Benefits, the value is always Price. The system calculates deductions for employees who select this option according to the deduction code linked to this benefit option. For Benefits Administration, the value can be Price or Credit. When you define a cost type as a credit, you must enter the appropriate earnings code. Use the earnings code to tell the system how to calculate the flexible credit earnings for a participant. Use a different earnings code for each benefit plan type within a benefit program. The system assigns the frequency of the additional pay based on the deduction code that you identify for this benefit option. |
|
Cost ID |
When you enter a new cost row, this value is assigned automatically by the system and cannot be updated. |
|
Rate Type |
Identifies the type of rate (flat amount, age-graded, and so on) associated with this plan type and benefit option combination. |
|
Rate TblID (rate table identification) |
Identifies which specific rate table is linked with this plan type and benefit option combination. You need the identification number because you may have established multiple tables for a particular rate type. Only plan types 01 through 3X can use rates. |
|
Earn Code |
Applies only to credits. Identifies the earning code that might be tied to the plan type. |
|
Calc TblID (calculation table identification) |
Identifies the calculation rule linked to the plan type and benefit option combination. |
Rate Availability by Plan Type
This table lists the rates types that you use for each plan type:
|
Plan Type |
Flat Rate |
Age-Graded |
Service Rate |
Percent of Salary |
|
01 |
For Benefit Administration only. |
For Benefit Administration only. |
For Benefit Administration only. |
For Benefit Administration only. |
|
1X |
Yes |
Yes |
Yes |
Yes |
|
2X |
Yes |
Yes |
Yes |
Yes |
|
3X |
Yes |
Yes |
Yes |
Yes |
|
4X−9X |
Not Used |
Not Used |
Not Used |
Not Used |
For some plan types, you will need to specify the proper Calculation Rules Table identification to ensure that the appropriate calculation rules are applied.
You don't have to indicate rates and calculation rules for all plan types. Certain rate types, on the other hand, require calculation rules.
Rate and Calculation Rule Requirements by Plan Type
This table lists the rate tables and calculation rules that you can use for different plan types:
|
Plan Type |
Rate Tables |
Calculation Rules Table |
|
01 |
Required |
Dependent on rate type. |
|
1x |
Required |
Required |
|
2x |
Required |
Required |
|
3x |
Required |
Required |
|
4x |
No |
Required |
|
5x |
No |
Required (reserved for future use), but not applied during calculations. |
|
6x |
No |
Not Used |
|
7x |
No |
Not Used |
|
8x |
No |
Not Used |
|
9x |
No |
Not Used |
Calculation Rule Requirements for Rate Types
Calculation rules are required for age-graded, flat-amount, salary-percentage, and service rate types.
 Cloning Benefit Programs, Eligibility Rules, or Event Rules
Cloning Benefit Programs, Eligibility Rules, or Event Rules
To clone a benefit program, use the Benefit Program Clone Utility (BN_CLONE) component.
This section discusses how to clone a benefit program.

 Page Used to Clone Benefit Programs, Eligibility Rules, or Event Rules
Page Used to Clone Benefit Programs, Eligibility Rules, or Event Rules|
Page Name |
Definition Name |
Navigation |
Usage |
|
BN_CLONE |
Set Up HRMS, Product Related, Base Benefits, Program Structure, Benefit Program Clone Utility, Benefit Program Clone Utility |
Clone a benefit program. Create a copy of an existing benefit program. Give the duplicated program a new effective date and choose whether to give the program a new name. Create a copy of an existing eligibility or event rule for Benefits Administration. |

 Cloning a Benefit Program
Cloning a Benefit Program
Access the Benefit Program Clone Utility page (Set Up HRMS, Product Related, Base Benefits, Program Structure, Benefit Program Clone Utility, Benefit Program Clone Utility).
|
Object Type to Clone |
Select an value: Benefit Program Eligibility Rule (Benefits Administration only) Event Rule (Benefits Administration only) |
|
Selected |
Select the check box for the object, benefit program, eligibility rule, or event rule that you want to clone. |
Copy To
This group box defines the name of the new object that will be created. These fields vary, depending upon the type of object you're cloning.