13 Process COBRA Notification
This chapter contains these topics:
-
Section 13.4, "Linking Dependents to a Qualified COBRA Beneficiary"
-
Section 13.8, "Reviewing Qualifying Events for a Beneficiary"
-
Section 13.9, "Reviewing the Report of Qualifying Events for a Beneficiary"
13.1 Processing COBRA Notification
You must notify all qualified beneficiaries when they become eligible for COBRA coverage. Current or terminated employees and their dependents become qualified beneficiaries for COBRA coverage when a qualifying event occurs. A qualifying event is any event, such as termination, that results in the loss of group health coverage for employees, their spouses, or dependents. Federal and state guidelines determine the duration of COBRA coverage based on the qualifying event.
When you notify qualified beneficiaries of their eligibility for COBRA coverage, you must notify them of the benefit plans and options that they have available and of the cost. Once notified, the qualified beneficiaries can elect COBRA coverage and submit the payment to your company each month for the duration of their coverage.
To process COBRA notification, complete the following tasks:
-
Entering COBRA Beneficiaries Manually
-
Entering COBRA Beneficiaries by Batch
-
Linking Dependents to a Qualified COBRA Beneficiary
-
Entering Qualifying Events
-
Creating COBRA Coverage
-
Preparing Coverage Information
-
Reviewing Qualifying Events for a Beneficiary
-
Reviewing the Report of Qualifying Events for a Beneficiary
13.2 Entering COBRA Beneficiaries Manually
From Human Resources (G08), choose COBRA Compliance
From COBRA Compliance (G08C1), choose Beneficiary Entry
You must enter each employee who becomes eligible for COBRA coverage as a qualified beneficiary. You must also enter the employee's dependents as qualified beneficiaries.
You can use this program to enter each qualified beneficiary manually. It is efficient to enter beneficiaries manually when you have only one or a few to enter. For example, a qualified beneficiary currently eligible for COBRA needs to add a new dependent as a beneficiary. Alternatively, you can enter qualified COBRA beneficiaries in one of the following ways:
| Method | Description |
|---|---|
| During employee entry | If you set the processing option, the system automatically adds all new employees to the COBRA Dependent/Beneficiary table as you enter each employee record.
When you use this method, you do not need to re-enter an individual when a qualifying event occurs. |
| With a batch process | If you have many employees to enter at one time, you can run a batch program that adds all the selected employee records to the COBRA Dependent/Beneficiary table. |
To enter qualified COBRA beneficiaries manually, complete one of the following tasks:
-
Enter a new COBRA beneficiary
-
Enter a current or former employee as a COBRA beneficiary
13.2.1 What You Should Know About
See Also:
-
Adding New Employees (P0801) in the JD Edwards World Human Resources Guide
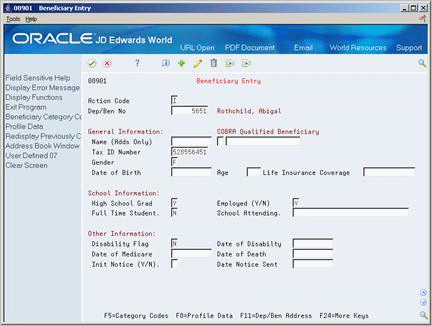
To enter a new COBRA beneficiary
On Beneficiary Entry
-
If you want to assign a specific number, complete the following field:
-
Dependent/Beneficiary Number
If you leave this field blank, the system assigns the next available number.
-
-
Complete the following field:
-
Name
-
-
Complete the following optional fields and use the Add action:
-
Tax ID number
-
Gender
-
Date of Birth
-
Disability Flag
-
Date of Disability
-
Date of Medicare
-
-
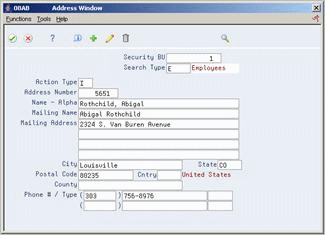
On Address Window, complete the following optional fields:
-
Search Type
-
Address
-
City
-
State
-
Postal Code
-
Phone Number
-
To enter a current or terminated employee as a COBRA beneficiary
On Beneficiary Entry
-
Enter the employee's number in the following field and press Enter:
-
Dependent/Beneficiary Number
-
-
Change any fields to update the record and press Enter.
-
On Address Window, update the beneficiary's address.
13.3 Entering COBRA Beneficiaries by Batch
From Human Resources (G08), choose COBRA Compliance
From COBRA Compliance (G08C1), enter 29
From COBRA Compliance Setup (G08C4), choose Create Beneficiaries from Employees
You must enter each employee as a qualified beneficiary who becomes eligible for COBRA coverage. You must also enter the employee's dependents as qualified beneficiaries. You can enter employees as qualified beneficiaries by batch before a qualifying event occurs. When the qualifying event occurs, you can retrieve the beneficiary information to notify the qualified beneficiaries that they are now eligible for COBRA coverage.
You can use this batch program to add all employee records to the COBRA Dependent/Beneficiary table at one time. Alternatively, you can enter beneficiaries in one of the following ways:
| Method | Description |
|---|---|
| During employee entry | If you set the processing option, the system automatically adds all new employees to the COBRA Dependent/Beneficiary table as you enter each employee record.
When you use this method, you do not need to re-enter an individual when a qualifying event occurs. |
| Manually | You can enter one beneficiary at a time. Use this method when you:
|
The system does not compile a report when you enter beneficiaries by batch.
See Also:
13.4 Linking Dependents to a Qualified COBRA Beneficiary
From Human Resources (G08), choose COBRA Compliance
From COBRA Compliance (G08C1), choose Dependents/Beneficiaries by EE
When you enroll a new employee in your benefit plans, you also enter the employee's dependents and link them to the employee's records. When the employee becomes eligible for COBRA coverage, the employee's dependents are also qualified beneficiaries. Occasionally, a qualified COBRA beneficiary needs to add a dependent as a qualified beneficiary who was not previously enrolled and linked. After you enter new individuals as a qualified COBRA beneficiaries, you must link them to employees or ex-employees. After you link them, they are eligible to receive benefits.
(Release A9.3 Update) Additionally, you can use the Enrollments List field to view only current enrollments or current and historical enrollments.
To link dependents to a qualified COBRA beneficiary
On Dependents and Beneficiaries by Employee
Figure 13-3 Dependents/Beneficiaries by EE screen
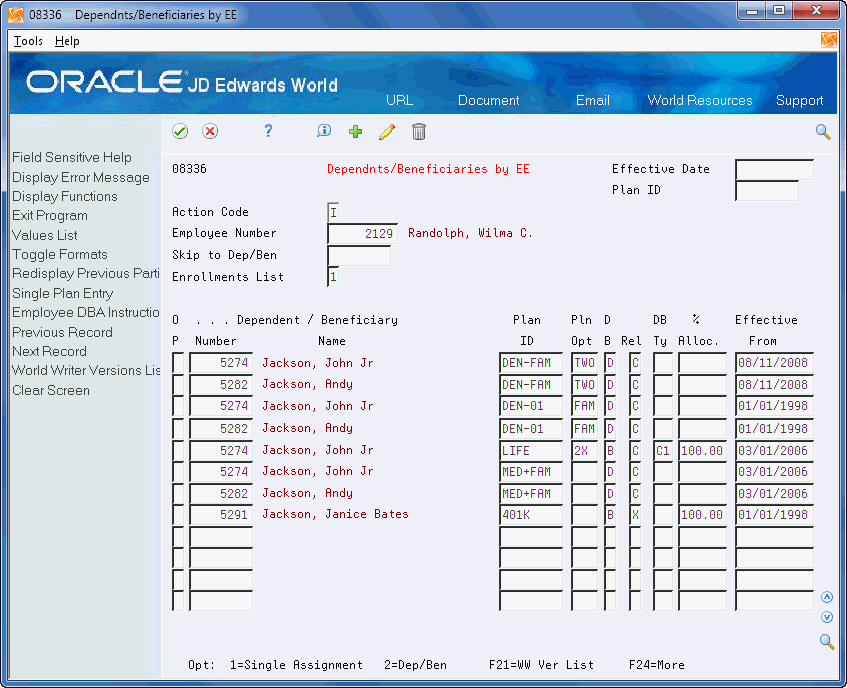
Description of "Figure 13-3 Dependents/Beneficiaries by EE screen"
13.5 Entering Qualifying Events
From Human Resources (G08), choose COBRA Compliance
From COBRA Compliance (G08C1), choose Enter QEs for Beneficiary
When a qualifying event occurs, qualified beneficiaries are eligible for COBRA coverage. A qualifying event is any event that results in the loss of group health coverage for employees, their spouses, or dependents. As part of the COBRA notification process, you must enter COBRA qualifying events for qualified beneficiaries.
The government mandates that you maintain and track important COBRA events. For example, you might record:
-
When the benefits administrator learns of the qualifying event
-
When you notified the qualified beneficiaries in writing
-
When the qualified beneficiary elected COBRA coverage
When you enter a qualifying event, the system does not automatically create the actual COBRA coverage but you can choose a function to create the COBRA coverage. If you do not want to create the coverage on the date you enter the qualifying event or if you are entering qualifying events for a large number of people, you might want to wait and create the coverage with a batch program.
When you enter a qualifying event for an existing employee, the system retrieves the benefit group or group plan information from the employee's master record. After you enter the qualifying event, the system maintains the information in the Qualifying Event for Beneficiary table (F08910).
13.5.1 Before You Begin
-
Ensure that the general constants for COBRA and qualifying events have been set up.
-
Ensure that the benefit group and plans for COBRA participants have been set up.
On Enter Qualifying Events for Beneficiary
Figure 13-4 Enter QEs for Beneficiary screen
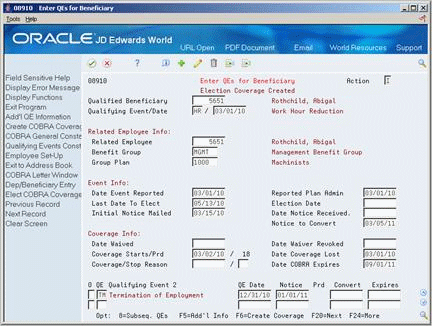
Description of "Figure 13-4 Enter QEs for Beneficiary screen"
-
Complete the following fields and press Enter:
-
Qualified Beneficiary
-
Qualifying Event
-
Qualifying Date
-
Date Event Reported
-
Reported Plan Administrator
The system enters the current plan information. It also calculates and enters other dates based on how the general and qualifying events constants are set up.
-
-
Review the information in the following fields:
-
Related Employee
-
Benefit Group
-
Group Plan
-
Last Date to Elect
-
Notice to Convert
-
Coverage Starts/Period
-
Date Coverage Lost
-
Date COBRA Expires
-
-
To print a letter for the qualified beneficiary, choose the Cobra Letter Window function.
-
On Cobra Letter Window, complete the following fields:
-
Document
-
Folder Name
-
-
Choose the Submit function.
-
Review the date in the following field:
-
Initial Notice Mailed
-
Last Date To Elect
-
-
If you want to create COBRA coverage for the qualified beneficiary, choose the Create Coverage function.
-
On the Create COBRA Coverage window, complete the following field:
| Field | Explanation |
|---|---|
| Qualified Beneficiary | The address number of the participant as defined in the Participant Master table (F08901).
In Dependent/Beneficiary Assignment, enter the participant number of the dependent/beneficiary who is being assigned to the benefit plan. In Qualifying Event Entry, enter the participant number of the qualified beneficiary who has lost coverage and is eligible to receive COBRA coverage. |
| COBRA Qualifying Event 1 | A user defined code (08/QE) that indicates the first (initial) event that qualified a participant for COBRA continuation. The coverage months are defined in the Qualifying Event Coverage Months table (F08990).
See also data item QET. |
| Date - Qualifying Event 1 | The date of the first (initial) qualifying event.
Form-specific information Enter the date that the event will occur. The system uses this date or the date coverage was lost to calculate the effective period for COBRA coverage. |
| Related Employee | The Address Book number of the employee through whom the qualified beneficiary receives benefits.
The system automatically brings in this number. |
| Date Event Reported | The date the COBRA event is first reported to the employer. |
| Reported Plan Admin | The date the COBRA event is first reported to the plan administrator. An employer has 30 days to report an employee's death, termination of employment, reduction in hours, or Medicare eligibility to the plan administrator. |
| Initial Notice Mailed | The date the election notice was mailed to the qualified beneficiary for the first qualifying event. The system automatically updates this date when you print the election form.
The system cannot create the COBRA coverage if this field is blank. The plan administrator must mail the notice within 14 days after being notified of the initial qualifying event. |
| Notice to Convert | The date plan administrators are required to notify all qualified beneficiaries of their right to convert to the current carrier providing coverage. This date is within 180 days of COBRA expiration. |
| Last Date To Elect | The last date that the participant can elect COBRA coverage.
Depending on the settings in the constants for the Election Period and Code fields, the specified election period is the latter of the following: 1 – Sixty days after the date plan coverage terminates 2 – Sixty days after the date that the plan administrator notifies the qualified beneficiary Form-specific information When you enter a value in the Initial Notice Mailed field, the system enters this date. |
| Coverage Starts/Prd | The date COBRA coverage begins.
The date that displays in this field depends on how you set the Use Loss of Coverage Date field in the COBRA Constants table (F08990). If you set the Use Loss of Coverage Date field to: Y – COBRA coverage begins the day after the date regular coverage was lost. N – COBRA coverage begins the day after the date of the qualifying event. |
| COBRA Coverage Period | The number of months that the qualified beneficiary is entitled to COBRA coverage. This number is generated by the system. |
| Date COBRA Expires | The date on which COBRA coverage expires. If you do not enter a date in this field, the system calculates the date by adding the number of months that COBRA coverage is effective (data item CVP) to the date regular coverage ends (data item DCLS).
If you do not enter the date regular on which coverage ends, the system uses the date of the qualifying event (data item QD1) as the begin date for coverage in this calculation. |
| Date Coverage Lost | The date that the participant lost regular coverage. If you do not enter a date in this field, the default value is the date of the qualifying event. |
| COBRA Folder | The name of the folder where COBRA notice documents are stored. Documents in this folder, such as initial COBRA notices and qualifying event notices, are sent to COBRA participants. |
| Documents | The name of the document titles for the various COBRA documents. |
13.5.2 What You Should Know About
13.6 Creating COBRA Coverage
From Human Resources (G08), choose COBRA Compliance
From COBRA Compliance (G08C1), choose COBRA Election Coverage
From COBRA Election Coverage (G08C11), choose Create Election Coverage
When you create COBRA coverage, the system analyzes the following information:
-
Qualifying event
-
Master plans for COBRA coverage
-
General constants for COBRA
-
Constants for qualifying events
Based on this information, the system compiles the benefit plans in which the qualified beneficiary can participate. It also compiles the costs the qualified beneficiary will incur when he or she elects to participate in the COBRA coverage. These costs can include the cost of the premium as identified in the rates and certain allowable administrative costs as identified in the constants.
After the system completes the processing, you can review the information online and print reports to send to each qualified beneficiary for which the system created coverage.
Use this program to create coverage for all qualified beneficiaries at one time, for example, when you have a lay-off. Companies with many employees use this method each week or pay period to ensure they create coverage for all terminated employees. Alternatively, you can create coverage for each qualified beneficiary when you enter the qualifying event for the employee.
13.6.1 Before You Begin
-
Verify that the benefit plan is entered in Plan Master Information and that it has been identified as a COBRA plan
-
Use the Plan Rates function from the employee DBA on the Plan Master to verify that COBRA rates are set up
-
Verify that the benefit plan is set up in Plans within Categories and that the category is attached to a benefit group
See Also:
-
Section 13.5.1, "Before You Begin"to alternatively create COBRA coverage for a qualified beneficiary when you enter the qualifying event
13.7 Preparing Coverage Information
From Human Resources (G08), choose COBRA Compliance
From COBRA Compliance (G08C1), choose COBRA Election Coverage
From COBRA Election Coverage (G08C11), choose Print Election Form
When employees leave the company, or another qualifying event occurs, you must notify them in writing that they are qualified beneficiaries and eligible to participate in COBRA coverage. After you enter the dates for the qualifying event and create COBRA coverage, you can print a report that lists the benefit plans included in the COBRA coverage and the costs associated with the plan.
When you use this program, the system generates an individual report based on the information it compiled when you created COBRA coverage. The report lists all the plans and options that the qualified beneficiary can elect. The report also includes the premiums and handling charges for the various plans. Qualified beneficiaries can use the report to indicate which plans they want to elect.
See Also:
-
Section 13.5.1, "Before You Begin" to print a letter that notifies qualified beneficiaries of the qualifying event
-
Section 24.2, "Setting Up a Plan Master for COBRA Coverage" to enter COBRA rates on a plan
13.8 Reviewing Qualifying Events for a Beneficiary
From Human Resources (G08), choose COBRA Compliance
From COBRA Compliance (G08C1), choose Review QEs for Beneficiary
You can review all qualifying events assigned to a qualified beneficiary after you create the coverage. The system retrieves information from the Participant table (F08901) and the COBRA Qualified Beneficiary table (F08910).
The system displays the initial qualifying event. Review qualifying events when you want to review one of the following:
-
Date that the initial qualifying event occurred
-
Last date that the qualified beneficiary can elect coverage
-
Date when COBRA coverage starts
You can access additional forms to review or add subsequent events, elections, or beneficiaries.
To review qualifying events for a beneficiary
Figure 13-5 Review QEs for Beneficiary screen
Description of "Figure 13-5 Review QEs for Beneficiary screen"
-
Complete the following field:
-
Dependent/Beneficiary
-
-
Choose the Qualifying Event option to access Enter Qualifying Events for Beneficiary.
13.9 Reviewing the Report of Qualifying Events for a Beneficiary
From Human Resources (G08), choose COBRA Compliance
From COBRA Compliance (G08C1), choose Print QEs for Beneficiary
The system retrieves the information from the COBRA Qualified Beneficiary table (F08910) to compile a report by qualified beneficiary. You can review information such as the following:
-
Qualified beneficiary name and address
-
Responsible party
-
Qualifying event and description
-
The date you printed the initial notification
-
All dates related to the qualifying event and COBRA coverage