Repository Model
This section describes the data model of the claim transaction repository. The claims transaction repository data model is based on the claims (working copy) data model. The main differences between the models are:
-
the transaction model includes additional financial transaction data that is added when creating claim transactions (for example, allocations to payment receivers),
-
the internal keys and references of the claims model are replaced with external meaningful values in the repository model,
-
some details of referenced entities are included in the repository model.
The repository claim transactions are in effect snapshots of claims and their referenced data at the time of finalization. Even though claims themselves are not versioned, claims transactions are versioned. Each time that a claim is finalized, a new claim transaction version is created in the repository.
See the Creation of a Transaction from a Claim - Example for an illustration of the differences between a claim transaction and a claim.
See the Claim Transaction Versioning Example for an illustration of versioning of claims in the transaction repository.
Design Principles
Minimal Validation
The transaction repository does not include referential integrity constraints other than those for internal use, for example, to implement internal master-detail relationships. Likewise, it does not enforce any business rules. The intention is that claim transactions are an accurate representation of the claim and referenced data at the time of finalization, even if aspects of this information are incorrect.
Transactions are Self Contained
As part of the creation of a claim transaction internal references from a claim (and its details) to other 'non-claim' entities are replaced with externally meaningful values from the data that is referenced within Claims (for example, internal ids are replaced with codes).
Within the repository itself, foreign keys are used to implement internal master / detail relationships. These are only used internally and are not included in any outbound messages. These internal foreign keys are resolved in the messages produced from the claims transaction repository by embedding the elements that represent the child objects within their parent elements. For example, even though coverages include a foreign key to their claim lines, the messages that deliver claims to external systems will have the coverages of a line as a list within the claim line element.
Included Referenced Data
In general, the referenced data that is included in the transaction repository is determined at the time that a transaction is created (that is, when the claim is finalized). For example, if some values are included in the repository from provider, the values would be as they are recorded for the provider at claim finalization time. If values are required as they were on another date (for example, claim service date), the dynamic logic of the transaction creation scenarios would need to specifically retrieve the value as it was at that the required time.
Multiple Language Considerations
Only the base language 'translation' of multi-language data will be included in the transaction repository. This is also the case with messages that can have substitution parameters. Messages will be included in the base language (with substitutions); however, the substitution parameters may also be stored with messages to provide the possibility for a downstream application to reconstruct the message in another language.
Basis of Entity Model
The data model of the transactions repository is based on the Claims entity model. The structure (attributes and associations between entities) are very similar to it. However, the transaction creation logic determines which attributes of the repository transactions are filled and the source of them. In general, it is expected that in most configurations the choice would be made to fill the transaction attributes directly from their corresponding Claims attributes. However, it is possible for different choices to be made. The 'Corresponding Claims Entity' column indicates the basis for repository fields and implicitly the expected / default source.
Preparation of the transaction creation logic is described in a separate section.
Dynamic Fields
Free fields and dynamic records can be added to each entity. Refer to the Repository Configuration section for more details.
Claim 'Unmatched' Attributes
The Claims data model includes attributes for holding values of related entities needed to match a claim to a related entity. These 'unmatched' attributes are not included as fixed fields in the repository as it is expected that by the time claims reach finalization matching will have occurred. If for some reason an 'unmatched' attribute is needed, it could be defined as a dynamic field.
Claim Line Internal Details
In the Claims entity model claim lines have several detail entities that are very specific to claims processing. These detail entities are not included in the transaction repository model as they are not seen as having meaning once a claim has been finalized. These internal detail entities are:
-
Limit Consumptions
-
Rule Coverages
-
Regime Consumptions
-
Authorization Consumptions
-
Case Details
These details could be added dynamic fields or records.
Data Types
In general, data types are carried through from the Claims data model. For example, dates will be stored as date fields even though they will primarily be sent out as strings.
Database Tables
The claim transaction repository is physically part of the Claims database. It is logically separate in the sense that it consists of an independent set of tables with no 'physical links' to the main claim tables (for example, they have no foreign keys to the main tables and no logic outside of the finalization step that accesses the repository tables directly).
Claim Versioning
Claims are considered to be a new version of an existing claim purely because they have the same claim code. The concept of claim versions is limited to the repository. Claims themselves do not have versions. Therefore, a claim version is in effect a 'count' of the number of times a claim with the same code has been finalized.
Versioning only applies at claim level. The claim lines (and other details) are not directly versioned by Claims. If claim lines need to be comparable between versions, it is up to the external components that send in new versions of claims to make sure that the claim lines can be recognized by their unique identification, that is, the combination of the claim code and the claim line code (unique within a claim).
Security
The downstream applications that receive / access information from the repository are treated as 'trusted' components in the overall SOA architecture. Security access restriction labels related to viewing claim information are included in the repository, and it is up to downstream applications to ensure that any restrictions that are needed based on them are implemented. Access restriction labels related to maintaining claim information (for example, adding and removing messages from claims or approving high-value claims) are not included as claims in the repository cannot be updated.
Data Model
The entities (and relationships) of the transaction repository are as illustrated here:
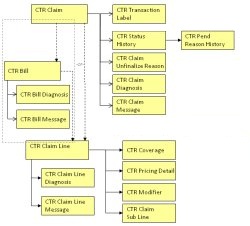
In addition to these entities, separate 'technical' entities are used to hold values of dynamic fields and records.
Corresponding Claims Entities
The details of each entity of the repository data model are described in the following sections. For each repository entity attribute, the corresponding Claims entity is indicated. For attributes that are from referenced entities where there is more than one relationship between the base entity and the referenced entity, the type of relationship is provided in italics. For example, Claimant Relation of Claim means that the attribute is from the relation with the 'claimant' relation type with the claim.
Descriptions of entities and attributes are not included. By default the meaning is the same as described for the corresponding Claims entities and attributes.
Dynamic logic determines the actual source of claim transaction values. Individual customers may choose different sources for claim transaction values than the indicated corresponding working copy entity.
Reversal Transactions
Reversal transactions are transactions with most amounts and numbers reversed (multiplied by -1). The Reverse? column in the table below indicates if a value is to be reversed in reversal transactions. Refer to Reversal Transactions section for more details.
Common Blocks of Attributes
Relation / Provider Details
Relation and provider details are included in the data model in several roles. For example, in claims, bills and claim lines relations are included in the 'payment receiver' role.
To reduce repetition, the inclusion of provider details is indicated in the format role + 'Provider Details'. This can be understood to mean that the following attributes are present prefixed with 'role name':
-
Provider Name
-
Provider Code
-
Provider Code Definition
The inclusion of relation details is indicated in the format role
'Relation Details'.
This can be understood to mean that the following attributes are present prefixed with 'role name':
-
Relation Name
-
Relation Code
CTR Claim
This entity is the 'header' of claim transactions.
| Corresponding Entity | Attribute | Reverse? | Note |
|---|---|---|---|
Claim |
Code |
||
None |
Version |
Set when transaction created. Simple increment of sequence within claim code. |
|
None |
Transaction Date |
Set to current date / time when transaction created. |
|
Claim |
Authorization Code |
||
Belongs to Brand of Claim |
Brand Code |
||
Belongs to Brand of Claim |
Brand Description |
||
has Access Restriction of Belongs to Brand of Claim |
Brand Access Restriction Code |
||
Belongs to Payer of Belongs to Brand of Claim |
Brand Payer Name |
||
has Access Restriction of Belongs to Payer of Belongs to Brand of Claim |
Brand Payer Access Restriction Code |
||
Grouped in Claim Set of Claim |
Claim Set Code |
||
Claim |
Claim Date |
||
Claimant Provider of Claim |
Claimant 'Provider Details' |
||
Claimant Relation of Claim |
Claimant 'Relation Details' |
||
has Access Restriction of Claimant Relation of Claim |
Claimant Access Restriction Code |
||
contact details Access Restriction of Claimant Relation of Claim |
Claimant Contact Details Access Restriction Code |
||
classified by Classification Scheme of Claim |
Classification Scheme Code |
||
has Classification of Claim |
Classification Code |
||
Claim |
Due Date |
||
Claim |
Emergency Indicator |
||
Claim |
End Date |
||
Claim |
Entry Date |
||
Claim |
Expiration Date |
||
Claim |
External Remarks |
||
Claim |
Ignore History Indicator |
||
Claim |
Internal Remarks |
||
Is of Claim Form |
Form Code |
||
Is of Claim Form |
Form Description |
||
Belongs to Data Access Group of Claim |
Data Access Group |
||
has Access Restriction of Belongs to Data Access Group of Claim |
Data Access Group Access Restriction Code |
||
Location Provider Provider of Claim |
Location 'Provider Details' |
||
Location Provider Provider of Claim |
Location Provider Address |
||
has Location Type of Claim |
Location Type Code |
||
has Location Type of Claim |
Location Type Description |
||
Claim |
Manual Indicator |
||
Claim |
Next Payer Code |
No look-up |
|
Claim |
Paid Date |
||
Destination Payer Payer Code of Claim |
Payer Code |
||
Payment Beneficiary Provider of Claim |
Payment Beneficiary 'Provider Details' |
||
Payment Beneficiary Relation of Claim |
Payment Beneficiary 'Relation Details' |
||
Payment Receiver Provider of Claim |
Payment Receiver 'Provider Details' |
||
Payment Receiver Relation of Claim |
Payment Receiver 'Relation Details' |
||
Payment Specification Receiver Provider of Claim |
Payment Specification Receiver 'Provider Details' |
||
Payment Specification Receiver Relation of Claim |
Payment Specification Receiver 'Relation Details' |
||
Claim |
Preceding Payer Code |
No look-up. |
|
Claim |
Price Date |
||
Claim |
Process Type |
C(laim) or R(eservation) |
|
Claim |
Provider Entity Reference |
||
Claim |
Provider Reference |
||
Claim |
Receipt Date |
||
Referral Provider Provider of Claim |
Referral 'Provider Details' |
||
None |
Reversal Indicator |
This field indicates if the transaction is a reversal transaction. |
|
Service Provider Provider of Claim |
Service 'Provider Details' |
||
Service Specialty Specialty of Claim |
Service Specialty Code |
||
Serviced Entity Relation of Claim |
Serviced Entity 'Relation Details' |
||
Serviced Entity Relation of Claim |
Serviced Entity Date |
||
Serviced Entity Relation of Claim |
Serviced Entity Date Interpretation |
||
has Access Restriction of Serviced Entity Relation of Claim |
Serviced Entity Access Restriction Code |
||
contact details Access Restriction of Serviced Entity Relation of Claim |
Serviced Entity Contact Details Access Restriction Code |
||
Claim |
Start Date |
||
Claim |
Total Allowed Amount |
Y |
|
uses (total allowed amount) Currency |
Total Allowed Amount Curr |
||
Claim |
Total Claimed Amount |
Y |
|
uses (total claimed amount) Currency |
Total Claimed Amount Curr |
||
Claim |
Total Covered Amount |
Y |
|
uses (total covered amount) Currency |
Total Covered Amount Curr |
||
Claim |
Type |
P(rovider) or R(estitution) |
CTR Transaction Labels
These labels provide additional information about a claim transaction that needs to be added after initial creation of a transaction. For now, they are only used to indicate that the claim of the transaction has been 'unfinalized'.
| Corresponding Entity | Attribute | Note |
|---|---|---|
None |
Label Date |
|
None |
Label Type |
CTR Status History
This entity holds the status history entries of claim transactions.
| Corresponding Entity | Attribute | Note |
|---|---|---|
Claim Status History |
Status |
|
Claim Status History |
Status Date |
CTR Pend Reason History
This entity holds the pend reason history entries for specific status history entries.
| Corresponding Entity | Attribute | Note |
|---|---|---|
Claim Pend Reason History |
Sequence |
|
Claim Pend Reason History |
Bill Provider Reference |
|
Claim Pend Reason History |
Resolved Datetime |
|
For Pend Reason of Claim Pend Reason History |
Code |
|
For Pend Reason of Claim Pend Reason History |
External Code |
|
For Pend Reason of Claim Pend Reason History |
Alternative Text |
|
For Pend Reason of Claim Pend Reason History |
Provider Text |
|
Resolved by User |
User Login Name |
CTR Callout History
This entity holds the callout history entries of claim transactions.
| Corresponding Entity | Attribute | Note |
|---|---|---|
Claim Callout History |
Request Sent Datetime |
|
Claim Callout History |
Response Received Datetime |
|
based on Callout Definition of Claim Callout Rule |
Code |
|
based on Callout Definition of Claim Callout Rule |
Description |
CTR Claim Unfinalize Reason
This entity holds the claim level unfinalize reasons of claim transactions.
| Corresponding Entity | Attribute | Note |
|---|---|---|
Claim Unfinalize Reason |
Source Reference |
|
Is unfinalized because of Unfinalize Reason of Claim Unfinalize Reason |
Code |
|
Is unfinalized because of Unfinalize Reason of Claim Unfinalize Reason |
External Code |
CTR Claim Diagnosis
This entity holds the claim level diagnoses of claim transactions.
| Corresponding Entity | Attribute | Note |
|---|---|---|
Applies To Diagnosis of Claim Diagnosis |
Code |
|
Applies To Diagnosis of Claim Diagnosis |
Code Definition |
|
Applies To Diagnosis of Claim Diagnosis |
Description |
|
Claim Diagnosis |
Sequence |
|
has Diagnosis Type of Claim Diagnosis |
Type Code |
|
has Diagnosis Type of Claim Diagnosis |
Type Description |
|
has Access Restriction of Applies To Diagnosis of Claim Diagnosis |
Access Restriction Code |
CTR Claim Message
This entry holds claim level messages of claim transactions.
| Corresponding Entity | Attribute | Note |
|---|---|---|
Knows Message of Claim Message of Claim |
Code |
|
Claim Message of Claim |
Origin |
|
None |
Message text with substituted parameters |
|
None |
Provider Message text with substituted parameters |
|
None |
Alternative Message text with substituted parameters |
|
Knows Message of Claim Message of Claim |
Severity |
|
Knows Message of Claim Message of Claim |
Priority |
|
Knows Message of Claim Message of Claim |
External Code |
|
Claim Message of Claim |
Overturned Indicator |
|
Knows User who overturned the Claim Message |
Login Name |
|
Claim Message of Claim |
Value 0 |
|
Claim Message of Claim |
Value 1 |
|
Claim Message of Claim |
Value 2 |
|
Claim Message of Claim |
Value 3 |
|
Claim Message of Claim |
Value 4 |
|
Claim Message of Claim |
Value 5 |
|
Claim Message of Claim |
Value 6 |
|
Claim Message of Claim |
Value 7 |
|
Claim Message of Claim |
Value 8 |
|
Claim Message of Claim |
Value 9 |
CTR Bill
This entity holds the bills of claim transactions.
| Corresponding Entity | Attribute | Note |
|---|---|---|
Bill |
Provider Reference |
|
Bill |
Provider Entity Reference |
Set when transaction created. |
Bill |
Bill Date |
|
Bill |
Authorization Code |
No look-up |
Bill |
Emergency Indicator |
|
Payment Receiver Provider of Bill |
Payment Receiver 'Provider Details' |
|
Payment Receiver Relation of Bill |
Payment Receiver 'Relation Details' |
|
Service Provider Provider of Bill |
Service 'Provider Details' |
|
Location Provider Provider of Bill |
Location 'Provider Details' |
|
has Location Type of Bill |
Location Type Code |
|
has Location Type of Bill |
Location Type Description |
|
Referral Provider Provider of Bill |
Referral 'Provider Details' |
|
Serviced Entity Relation of Bill |
Serviced Entity 'Relation Details' |
|
Serviced Entity Relation of Bill |
Serviced Entity Date |
|
Serviced Entity Relation of Bill |
Serviced Entity Date Interpretation |
|
has Access Restriction of Serviced Entity Relation of Bill |
Serviced Entity Access Restriction Code |
|
contact details Access Restriction of Serviced Entity Relation of Bill |
Serviced Entity Contact Details Access Restriction Code |
|
Service Specialty Specialty of Bill |
Service Specialty Code |
CTR Bill Diagnosis
This entity contains the diagnoses of bills.
| Corresponding Entity | Attribute | Note |
|---|---|---|
Applies To Diagnosis of Bill Diagnosis |
Code |
|
Applies To Diagnosis of Bill Diagnosis |
Code Definition |
|
Applies To Diagnosis of Bill Diagnosis |
Description |
|
Bill Diagnosis |
Sequence |
|
has Diagnosis Type of Bill Diagnosis |
Type Code |
|
has Diagnosis Type of Bill Diagnosis |
Type Description |
|
has Access Restriction of Applies To Diagnosis of Bill Diagnosis |
Access Restriction Code |
CTR Bill Message
This entity contains the messages of bills.
| Corresponding Entity | Attribute | Note |
|---|---|---|
Knows Message of Bill Message of Bill |
Code |
|
Bill Message of Bill |
Origin |
|
None |
Message text with substituted parameters |
|
None |
Provider Message text with substituted parameters |
|
None |
Alternative Message text with substituted parameters |
|
Knows Message of Bill Message of Bill |
Severity |
|
Knows Message of Bill Message of Bill |
Priority |
|
Knows Message of Bill Message of Bill |
External Code |
|
Claim Message of Claim |
Value 0 |
|
Bill Message of Bill |
Value 1 |
|
Bill Message of Bill |
Value 2 |
|
Bill Message of Bill |
Value 3 |
|
Bill Message of Bill |
Value 4 |
|
Bill Message of Bill |
Value 5 |
|
Bill Message of Bill |
Value 6 |
|
Bill Message of Bill |
Value 7 |
|
Bill Message of Bill |
Value 8 |
|
Bill Message of Bill |
Value 9 |
CTR Claim Policy Product
This entity holds the policy product details of the claim that is obtained through enrollment callout.
| Corresponding Entity | Attribute | Note |
|---|---|---|
Specifies Product of Policy Product |
Code |
|
has Insurable Entity of Policy Product |
Serviced Entity Type |
|
has Insurable Entity of Policy Product |
Serviced Entity Code |
|
is employed by Organization |
Organization Code |
|
Policy Product |
Start Date |
|
Policy Product |
End Date |
|
Policy Product |
Subscription Date |
|
Policy Product |
Subscription End Date |
|
Group Account Code |
Dynamic field on Policy Product |
|
Enrollment Product Code |
Dynamic field on Policy Product |
|
Add-on Code |
Dynamic field on Policy Product |
Note: During implementation, if policy product information is required in CTR for any downstream processing, then Claims recommends using this entity for that purpose. Also, note that for Product Profitability analysis (for example, covered amount vs premium paid for a group account), Oracle Health Insurance Analytics uses enrollment product, add-on and group account details from this entity.
CTR Claim Line
This entity holds the claim lines of claim transactions or bills.
| Corresponding Entity | Attribute | Reverse? | Note |
|---|---|---|---|
Claim Line |
Code |
||
Claim Line |
Sequence |
||
Claim Line |
Allowed Amount |
Y |
|
uses (allowed amount) Currency |
Allowed Amount Curr |
||
Claim Line |
Allowed Number of Units |
Y |
|
Claim Line |
Authorization Code |
||
Claim Line |
Authorization Exception Type |
||
Overriding Authorization Regime of Claim Line Override |
Authorization Regime Code |
||
Overriding Coverage Specification of Claim Line Override |
Coverage Specification Code |
||
Benefits Provider Provider of Claim Line |
Benefits Provider 'Provider Details' |
||
Claim Line |
Benefits Age Input Date |
||
Claim Line |
Benefits Input Amount |
Y |
|
uses (benefits input amount) Currency |
Benefits Input Amount Curr |
||
Claim Line |
Benefits Input Date |
||
using reservation of Claim Line |
Reservation Code |
||
using reservation of Claim Line |
Reservation Line Code |
||
Claim Line |
Claimed Amount |
Y |
|
uses (claimed amount) Currency |
Claimed Amount Curr |
||
Claim Line |
Claimed Number Of Units |
Y |
|
has Classification of Claim Line |
Classification Code |
||
is classified on grounds of Authorization of Claim Line |
Class Authorization Code |
||
Overriding Coverage Regime of Claim Line |
Coverage Regime Code |
||
Overriding Coverage Regime (No auth. found) of Claim Line Override |
Coverage Regime No Auth Code |
||
Claim Line |
Covered Amount |
Y |
|
uses (covered amount) Currency |
Covered Amount Curr |
||
Claim Line |
Covered Number of Units |
Y |
|
Claim Line |
Encounter Indicator |
||
Claim Line |
Emergency Indicator |
||
Claim Line |
End Date |
||
Claim Line |
Family Code |
||
Overriding Funding Arrangement of Claim Line Override |
Funding Arrangement Code |
||
Location Provider Provider of Claim Line |
Location 'Provider Details' |
||
has Location Type of Claim Line |
Location Type Code |
||
has Location Type of Claim Line |
Location Type Description |
||
Payment Receiver Provider of Claim Line |
Payment Receiver 'Provider Details' |
||
Payment Receiver Relation of Claim Line |
Payment Receiver 'Relation Details' |
||
Overriding Post Benefit Regime of Claim Line Override |
Post Benefit Regime Code |
||
Claim Line |
Preceding Payer Paid Amount |
Y |
|
uses (preceding payer paid amount) Currency |
Preceding Payer Paid Amount Curr |
||
Claim Line |
Price Input Date |
||
Claim Line |
Price Input Number of Units |
Y |
|
Individual Price Provider Provider of Claim Line |
Price Individual Provider 'Provider Details' |
||
Organization Price Provider Provider of Claim Line |
Price Organization Provider 'Provider Details' |
||
Claim Line |
Price Principal Proc1 Ind |
||
Claim Line |
Price Principal Proc2 Ind |
||
Claim Line |
Price Principal Proc3 Ind |
||
Specifies Procedure of Claim Line |
Procedure Code |
||
Specifies Procedure of Claim Line |
Procedure Definition |
||
Specifies Procedure of Claim Line |
Procedure Description |
||
Specifies Procedure 2 of Claim Line |
Procedure 2 Code |
||
Specifies Procedure 2 of Claim Line |
Procedure 2 Definition |
||
Specifies Procedure 2 of Claim Line |
Procedure 2 Description |
||
Specifies Procedure 3 of Claim Line |
Procedure 3 Code |
||
Specifies Procedure 3 of Claim Line |
Procedure 3 Definition |
||
Specifies Procedure 3 of Claim Line |
Procedure 3 Description |
||
has Access Restriction of Specifies Procedure of Claim Line |
Procedure Access Restriction Code |
||
has Access Restriction of Specifies Procedure 2 of Claim Line |
Procedure 2 Access Restriction Code |
||
has Access Restriction of Specifies Procedure 3 of Claim Line |
Procedure 3 Access Restriction Code |
||
Claim Line |
Process as IN |
||
Overriding Product of Claim Line Override |
Product Code |
||
Overriding Product Family of Claim Line Override |
Product Family Code |
||
Overriding Product Line of Claim Line Override |
Product Line Code |
||
Claim Line |
Provider Entity Reference |
||
Claim Line |
Provider Reference |
||
Referral Provider Provider of Claim Line |
Referral Provider 'Provider Details' |
||
Claim Line |
Replaced Indicator |
||
Original For Claim Line of Claim Line |
Replaced by Code |
||
Replacement Of Claim Line of Claim Line |
Replaces Code |
||
Claim Line |
Reservation Code |
||
Service Provider Provider of Claim Line |
Service 'Provider Details' |
||
Service Specialty Specialty of Claim Line |
Service Specialty Code |
||
Serviced Entity Relation of Claim Line |
Serviced Entity 'Relation Details' |
||
Serviced Entity Relation of Claim Line |
Serviced Entity Date |
||
Serviced Entity Relation of Claim Line |
Serviced Entity Date Interpretation |
||
has Access Restriction of Serviced Entity Relation of Claim Line |
Serviced Entity Access Restriction Code |
||
contact details Access Restriction of Serviced Entity Relation of Claim Line |
Serviced Entity Contact Details Access Restriction Code |
||
Claim Line |
Start Date |
||
Claim Line |
Status |
||
Claim Line |
Subscription Date |
||
Claim Line |
Waiting Period Input Date |
||
Overriding Waiting Period Regime of Claim Line Override |
Waiting Period Regime Code |
CTR Claim Line Diagnosis
This entity holds the diagnoses of claim lines.
| Corresponding Entity | Attribute | Note |
|---|---|---|
Applies To Diagnosis of Claim Line Diagnosis |
Code |
|
Applies To Diagnosis of Claim Line Diagnosis |
Code Definition |
|
Applies To Diagnosis of Claim Line Diagnosis |
Description |
|
Claim Line Diagnosis |
Sequence |
|
has Diagnosis Type of Claim Line Diagnosis |
Type Code |
|
has Diagnosis Type of Claim Line Diagnosis |
Type Description |
|
has Access Restriction of Applies To Diagnosis of Claim Line Diagnosis |
Access Restriction Code |
CTR Claim Line Message
This entity holds the messages of claim lines.
| Corresponding Entity | Attribute | Note |
|---|---|---|
Knows Message of Claim Line Message of Claim Line |
Code |
|
Claim Line Message of Claim Line |
Origin |
|
None |
Message text with substituted parameters |
|
None |
Provider Message text with substituted parameters |
|
None |
Alternative Message text with substituted parameters |
|
Knows Message of Claim Line Message of Claim Line |
Severity |
|
Knows Message of Claim Line Message of Claim Line |
Priority |
|
Knows Message of Claim Line Message of Claim Line |
External Code |
|
For Product of Claim Line Message of Claim Line |
Product Code |
|
Claim Line Message of Claim Line |
Overturned Indicator |
|
Knows User who overturned the Claim Line Message |
Login Name |
|
Claim Line Message of Claim Line |
Value 1 |
|
Claim Line Message of Claim Line |
Value 2 |
|
Claim Line Message of Claim Line |
Value 3 |
|
Claim Line Message of Claim Line |
Value 4 |
|
Claim Line Message of Claim Line |
Value 5 |
|
Claim Line Message of Claim Line |
Value 6 |
|
Claim Line Message of Claim Line |
Value 7 |
|
Claim Line Message of Claim Line |
Value 8 |
|
Claim Line Message of Claim Line |
Value 9 |
CTR Claim Line Coverage
This line hold coverages of claim lines.
| Corresponding Entity | Reverse? | Note | |
|---|---|---|---|
Claim Line Coverage |
Action |
||
Claim Line Coverage |
Display Name |
||
Claim Line Coverage |
Amount |
Y |
|
uses for amount Currency |
Amount Curr |
||
Claim Line Coverage |
Number |
Y |
|
By Product of Claim Line Coverage |
Product Code |
||
By Product of Claim Line Coverage |
Product Description |
||
By Product of Carried By Brand of Claim Line Coverage |
Product Brand Code |
||
By Product of Carried By Brand of Claim Line Coverage |
Product Brand Description |
||
By Product of Carried By Family of Claim Line Coverage |
Product Family Code |
||
Has Coverage Label of Claim Line Coverage |
Coverage Label Code |
||
Has Coverage Label of Claim Line Coverage |
Coverage Label Display Sequence |
CTR Claim Line Contract Reference
This entity holds contract references that apply to claim lines.
| Corresponding Entity | Attribute | Note |
|---|---|---|
has Claim Line Contract Reference |
Code |
|
has Claim Line Contract Reference |
Description |
CTR Claim Line Modifier
This entity holds modifiers of claim lines.
| Corresponding Entity | Attribute | Note |
|---|---|---|
Is Of Type Claim Line Modifier |
Code |
|
Is Of Type Claim Line Modifier |
Description |
CTR Claim Line Benefit Specification
This entity holds details about the benefit specifications that have been applied in the benefits calculation of claim lines.
| Corresponding Entity | Attribute | Note |
|---|---|---|
uses Benefit Specification of Claim Line Benefit Specification |
Benefit Specification Code |
|
uses Benefit Specification of Claim Line Benefit Specification |
Benefit Specification Subtype |
|
uses Coverage Regime / Authorization Regime / Waiting Period Regime of Claim Line Benefit Specification |
Regime Code |
|
for Product of Claim Line Benefit Specification |
Product Code |
|
Claim Line Benefit Specification |
Product Provider Group Status |
|
uses product Provider Group of Claim Line Benefit Specification |
Product Provider Group Code |
|
Claim Line Benefit Specification |
Specific Provider Group Status |
|
uses specific Provider Group of Claim Line Benefit Specification |
Specific Provider Group Code |
|
Claim Line Benefit Specification |
Inherited Provider Group Status |
|
Claim Line Benefit Specification |
Processed as In |
CTR Claim Line Provider Pricing Clause
This entity holds details about the provider pricing clauses that have been applied in the pricing of claim lines.
| Corresponding Entity | Attribute | Reverse | Note |
|---|---|---|---|
Claim Line Provider Pricing Clause |
Sequence |
||
uses Reimbursement Method / uses Pricing Rule |
Type |
Fee Schedule / Charged Amount / Payment System / Adjustment / Carve Out / Dynamic Field / Encounter / Lower Of / Message / Provider Limit / External Intervention |
|
uses Provider Pricing Clause |
Description |
||
uses Provider Pricing Clause |
Quantifier |
The quantifier of the provider pricing clause, which can be either a percentage, maximum amount, maximum number of units or maximum service days |
|
uses Reimbursement Method / uses Pricing Rule |
Code |
||
Claim Line Provider Pricing Clause |
Amount |
Y |
|
uses for amount Currency |
Amount Curr |
||
Claim Line Provider Pricing Clause |
Mark |
| For a claim line provider pricing clause, either the type and code of a reimbursement method are stored or the type and code of a pricing rule. This is because a provider pricing clause either uses a reimbursement method or a pricing rule. |
CTR Claim Line Applied Parameter
This entity holds details about the parameter and limit values that were actually applied on the claim line during the claims flow.
| Corresponding Entity | Attribute | Reverse | Note |
|---|---|---|---|
Claim Line Applied Parameter |
Percentage |
||
Claim Line Applied Parameter |
Amount per Unit |
||
uses for amount |
Amount per Unit Currency |
||
in context of |
Benefit Specification Code |
||
in context of |
Product Code |
||
for |
Cover Withhold Category Code |
||
uses for max amount |
Maximum Amount Currency |
||
Claim Line Applied Parameter |
Maximum Service Days |
||
Claim Line Applied Parameter |
Maximum Number |
||
Claim Line Applied Parameter |
Maximum Amount |
||
Claim Line Applied Parameter |
Alias Code |
||
for Limit |
Limit Code |
||
Claim Line Applied Parameter |
Reached Action |
CTR Claim Sub Line
This entity holds claim sub lines of claim lines.
| Corresponding Entity | Attribute | Reverse? | Note |
|---|---|---|---|
Claim Sub Line |
Sequence |
||
Claim Sub Line |
Claimed Number of Units |
Y |
|
Specifies Procedure of Claim Sub Line |
Procedure Code |
||
Specifies Procedure of Claim Sub Line |
Procedure Code Definition |
||
has Access Restriction of Specifies Procedure of Claim Sub Line |
Procedure Access Restriction Code |