Manual Adjudication of a Claim
If the evaluation of external intervention rules in the manual adjudication step of the process flow pends a claim, the claim requires manual adjudication. See Manual Adjudication for more information on manual adjudication as part of the process flow.
This page describes manual adjudication through the Oracle Health Insurance Claims Adjudication and Pricing JET UI.
Oracle Health Insurance only allows manual adjudication of claims that have the status MANUAL ADJUDICATION [1].
Page Appearance
The page is display only, except for claim and claim line pend reasons, claim messages, claim notes, external data, and financial holds.
Claim
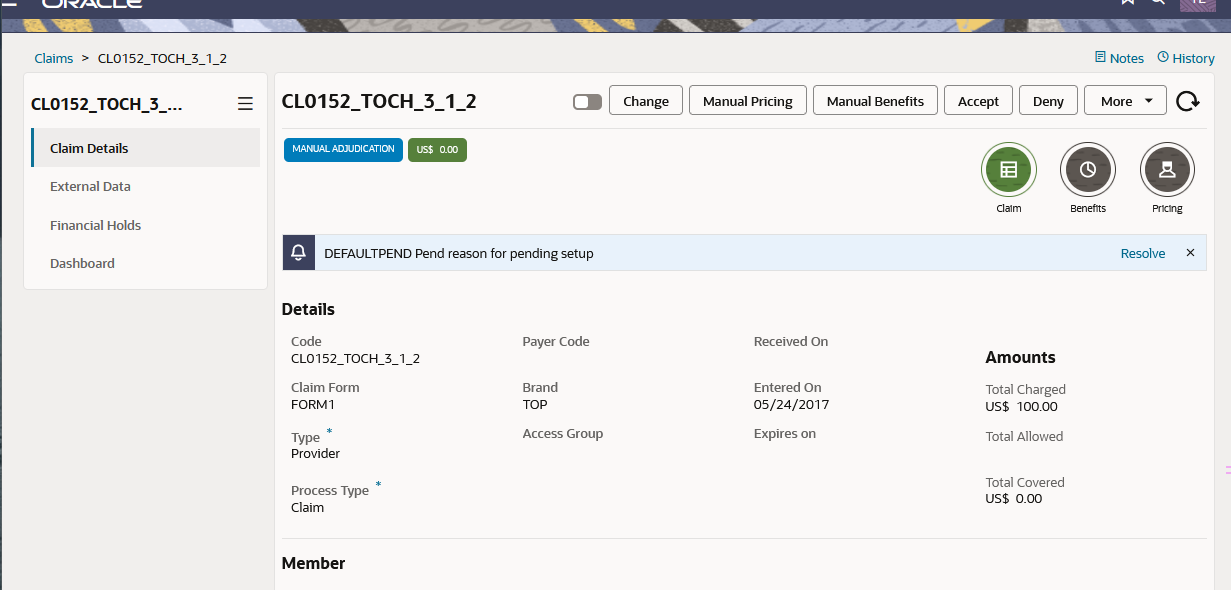
The user can perform one of the following actions:
Change
The system reverts the claim to the CHANGE status. This makes it possible to change the claim, for example, changing the serviced person. [2]
This action uses the Back to Change http operation.
Manual Pricing
The system reverts the claim to the MANUAL PRICING status. This makes it possible to change the pricing results on the claim lines. [2]
This action uses the Back to Manual Pricing http operation.
Manual Benefits
The system reverts the claim to the MANUAL BENEFITS status. This makes it possible to change the benefits results on the claim lines. [2]
This action uses the Back to Manual Benefits http operation.
Accept
The system submits the claim for re-processing.
This action uses the Submit Operation http operation.
Deny
The system prompts the user to select a fatal message that is to be attached to the claim. When the user saves the message, the system automatically applies a list of updates to the claim and submits the claim for re-processing.
Claim Details
The claim’s details are divided over the sections Claim, Benefits and Pricing. If the claim has unfinalize reasons they display in a separate section.
The top of the claim section displays pend reasons, messages and errors attached to this version of the claim.
For more information on these claim details see Claim details.
Claim Line
The user can perform one of the following actions on one or more claim lines.
Resolve Pend Reason
The system prompts the user to select a pend reason[3] and resolves the selected pend reason on all the claim lines where that pend reason exists. The system re-processes the claim.
This action uses the Resolve Pend Reasons http operation.
More
The More button enables the user to add a message, remove a message or add a pend reason to the selected claim lines.
The system prompts the user to select a message[4] or a pend reason.
After selecting the message or pend reason the system responds with an overview of the additions or removals it will do, and prompts the user to confirm (Submit).
Submitting the changes triggers a recalculation of the claim and refreshes the content of the page.
… Open
The Open option opens the claim line in a separate claim line window. In this window the user can deny the claim line and resolve claim line pend reasons.
…Deny
The Deny option prompts the user to select a fatal message. After selecting, the system adds the message to the claim line and sets the status of the claim line to 'DENIED'.
The system prompts the user to select a fatal message that is to be attached to the claim. See Adding a Fatal Claim Line Message for the updates the system applies when denying a claim line.
It is not possible to deny a claim line if the claim line:
-
is locked
-
is replaced
-
has a fatal product-independent message attached
-
has a fatal product-dependant message attached, but one or more claim line rule coverages exist
Denying a single claim line may affect the adjudication of other approved lines in the same claim.
When the user saves the message, the system automatically applies a list of updates to the claim line and submits the claim for re-processing.
The Claim Line’s TO BE Label
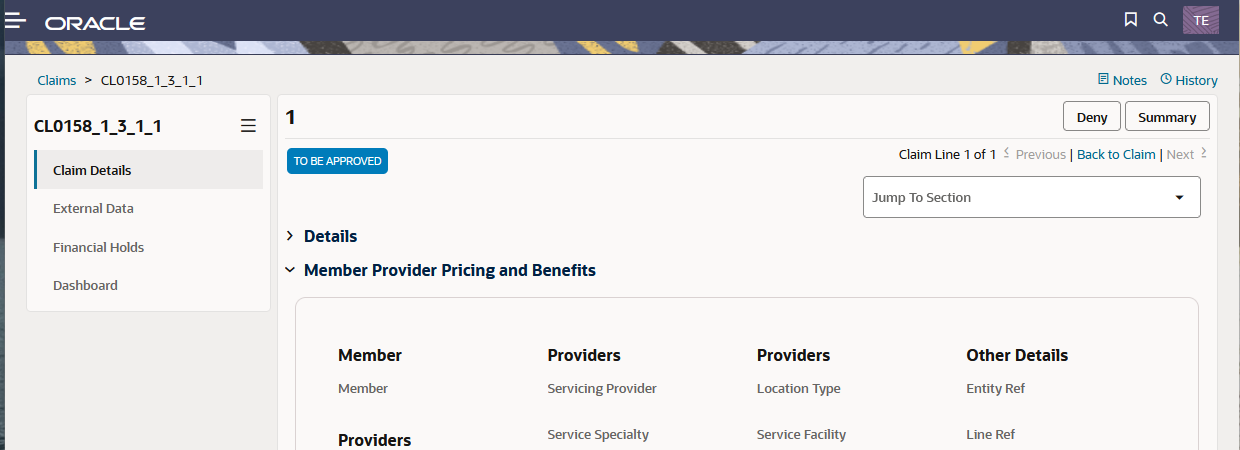
The TO BE label on the claim line gives a forecast of the claim line status for non-replaced claim lines and non-locked claim lines in the event that the claim is accepted.
Since the claim line status is not set for claims in the status MANUAL ADJUDICATION, the value of this label is derived.
If the claim line meets at least one of the following conditions:
-
the claim to which the claim line belongs has a fatal message attached;
-
the claim line itself has a non-product-specific fatal message attached;
then the claim line "TO BE" label is "TO BE DENIED". The claim line will be denied once the claim is submitted.
Otherwise, the label is set to "TO BE APPROVED". The claim line will be approved once the claim is submitted.